Quote:
Originally Posted by Tupelo3
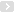
Intranasal delivery directly targets the brain, does not require surgery, and could be used in patients ineligible for surgery.
The intranasal route bypasses the BBB. Only a small percentage of the administered dose reaches the brain, but small amounts of GDNF may be sufficient (due to its high potency on dopamine neurons), and desirable (due to side-effects associated with too much GDNF in brain).
Intranasal delivery limits distribution outside the brain, and therefore limits potential side-effects in other tissues, an advantage over intravenous administration.
Copernicus plasmid DNA nanoparticles successfully transfect cells in the brain after nasal delivery, making them capable of producing GDNF within the brain - Copernicus DNA nanoparticles are safe and non-immunogenic. They have been given via the nose for other applications, such as to deliver the gene for cystic fibrosis to the lungs
- AAV vectors can be immunogenic and they integrate into the host cell DNA, so production is lasting and hard to regulate.
- Plasmid DNA does not integrate with the host cell DNA, so transfection is time limited
- GDNF production is scalable, and nasal re-dosing is possible and easy. If adverse effects develop, dosing could be terminated and production would eventually stop.
- The time course of GDNF production can be modified by design of the plasmid
- The time course of production still needs to be determined for intranasal pGDNF NPs. New funding is sought for this work.
- Dose-response relationships must be determined to see if giving more yields proportionally more GDNF production. Funding is also sought for this
Dr. Waszczak's Progress and future plans:
Research in the Waszczak lab has shown that intranasal pGDNF NPs significantly reduce dopamine cell loss in the rat 6-OHDA model of Parkinsons disease.
The next step (after time course and dose-response studies in rats) is testing in a large brain primate to determine if intranasal pGDNF NPs are likely to work in humans. A major grant from the NIH (or other source) will be needed.
If the primate study is promising, Copernicus and Northeastern University will pursue an IND for a clinical trial. Funding prospects uncertain.
MRI-guided focused ultrasound (FUS) may enrich delivery of intranasal pGDNF NPs to the target brain areas (substantia nigra and striatum).
o FUS is non-invasive; it is a brief, focused application of low energy sonication to areas where pGDNF NP delivery is desired. FUS would be done just before or after the intranasal dose is given.
o A new grant awarded to the Waszczak lab and collaborators at Harvard Medical School and Copernicus Therapeutics will allow us to investigate whether FUS increases delivery to the target brain areas. |
Expression of GDNF Throughout Rat Brain After Intranasal Delivery of hGDNF Plasmid Nanoparticles
http://www.fasebj.org/content/29/1_S...20.10.abstract